Is dysautonomia disabling?
 Dysautonomia can indeed be disabling, as it encompasses a group of disorders that affect the autonomic nervous system, which controls many vital bodily functions. The severity of dysautonomia symptoms can vary from person to person, but in more severe cases, they can significantly impair your ability to maintain gainful employment. However, whether your dysautonomia symptoms result in disability depends on the specific type and severity of your condition.
Dysautonomia can indeed be disabling, as it encompasses a group of disorders that affect the autonomic nervous system, which controls many vital bodily functions. The severity of dysautonomia symptoms can vary from person to person, but in more severe cases, they can significantly impair your ability to maintain gainful employment. However, whether your dysautonomia symptoms result in disability depends on the specific type and severity of your condition.
What conditions cause dysautonomia?
Dysautonomia is a term that refers to a group of disorders characterized by dysfunction of the autonomic nervous system, which controls automatic bodily functions such as heart rate, blood pressure, digestion, and temperature regulation. There are various conditions and factors that can lead to or be associated with dysautonomia, including:
-
- Postural Orthostatic Tachycardia Syndrome (“POTS”);
- Pure Autonomic Failure (“PAF”);
- Multiple System Atrophy (“MSA”);
- Neurological disorders such as Parkinson’s disease and neuropathies, which can damage the autonomic nervous system and cause dysautonomia as a secondary symptom;
- Ehlers-Danlos Syndrome (“EDS”), a condition causing hypermobility of the joints and connective tissue, which can affect the autonomic nervous system and result in dysautonomia;
- Long Covid;
- Diabetes, which may cause neuropathy that can damage nerves, including those in the autonomic nervous system, and lead to autonomic dysfunction and dysautonomia;
- Autoimmune disorders, such as autoimmune autonomic ganglionopathy, can result in the immune system mistakenly attacking the autonomic nervous system, leading to dysautonomia;
- Lyme disease and Babesiosis can cause damage to the autonomic nerves and result in dysautonomia;
- Physical trauma, such as spinal cord injuries, can disrupt the autonomic nervous system and lead to autonomic dysfunction.
- Exposure to certain toxins or chemicals can damage nerves, including those of the autonomic nervous system, causing dysautonomia.
Dysautonomia can manifest in different ways and with varying severity depending on the underlying cause. Additionally, some cases of dysautonomia may not have a known cause and are classified as idiopathic.
Regardless of cause, the impact of dysautonomia on daily life can be profound and may lead to long term disability. It can result in significant limitations in both physical and cognitive functioning. To evaluate the long term disability caused by dysautonomia effectively, it’s crucial to consider the overall impact, including the frequency and severity of the symptoms.
What are the disabling symptoms of dysautonomia?
Dysautonomia results in an array of potentially disabling symptoms, both physical and cognitive. During symptom flare-ups or episodes of autonomic dysfunction, these symptoms can be especially severe.
Disabling physical symptoms of dysautonomia may include:
-
- Orthostatic intolerance, causing difficulty standing for extended periods or experience dizziness, lightheadedness, and even fainting upon standing;
- Tachycardia (abnormally fast heartrate) or Bradycardia (slow heart rate), both of which can result in discomfort, fatigue, or fainting;
- Blood pressure fluctuations, where blood pressure may drop upon standing (known as orthostatic hypotension) or spike unpredictably, leading to dizziness, blurred vision, and in some cases, fainting;
- Chronic fatigue, often exacerbated by the effort required to manage your symptoms;
- Muscle weakness and pain, resulting from prolonged periods of inactivity due to fatigue or difficulty moving;
- Temperature regulation issues, leading to excessive sweating, heat intolerance, or cold extremities;
- Visual disturbances, including blurry vision or even temporary blindness upon standing, a condition known as visual disturbances during orthostatic stress;
Disabling cognitive and emotional symptoms of dysautonomia may include:
-
- Brain fog;
- Memory problems;
- Mental fatigue, making it challenging to perform tasks that require sustained concentration; and
- Anxiety and depression, arising from the chronic nature of dysautonomia and the uncertainty of symptom fluctuations, which can further impair cognitive function.
Can I get long term disability benefits for dysautonomia?
Yes, it is possible to receive long term disability benefits for dysautonomia. However, whether you are eligible for benefits will depend on the terms of your insurance policy and the nature of your symptoms.
Disability insurance policies have their own definitions for what constitutes a disability. It’s essential to review your disability insurance policy to understand the specific terms and conditions for making a claim. Your policy will outline the criteria you must meet for disability, waiting periods, and other requirements.
The severity of your dysautonomia symptoms will also play a crucial role in determining your eligibility for benefits. Your insurer will generally assess how your dysautonomia impacts your functioning in relation to work-related tasks. In order to approve your claim, your insurer will require you to comprehensively demonstrate how your dysautonomia interferes with your ability to work.
This requirement can be challenging if you have dysautonomia. Dysautonomia symptoms often fluctuate and vary widely among individuals, making it hard to document and establish consistent limitations for work-related tasks. Many of these symptoms are also not visible, and there are few clear-cut, objective tests that definitively confirm dysautonomia. These factors can lead to skepticism from your insurer and difficulties in convincing them of the disabling nature of your condition.
Below we’ll explain what evidence you may submit to support your dysautonomia long term disability claim.
What evidence can prove dysautonomia as a disability?
 When applying for long term disability due to dysautonomia, your insurer will require you to provide comprehensive evidence of your condition to support your claim. The specific medical evidence for dysautonomia can vary depending on the type and suspected underlying causes.
When applying for long term disability due to dysautonomia, your insurer will require you to provide comprehensive evidence of your condition to support your claim. The specific medical evidence for dysautonomia can vary depending on the type and suspected underlying causes.
Here are some examples of medical and vocational evidence you may use to support your dysautonomia long term disability claim:
-
- Tilt Table Test, autonomic function testing which is often used to diagnose conditions like postural orthostatic tachycardia syndrome (“POTS”);
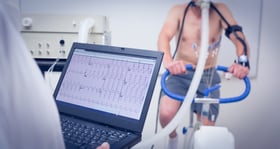
- Cardiopulmonary Exercise Test (“CPET”), a diagnostic evaluation that measures your cardiovascular and respiratory responses to physical exertion and can assess functional limitations and capabilities, helping to substantiate your long term disability claim for dysautonomia;
- Quantitative Sudomotor Axon Reflex Test (“QSART”), which measures sweat gland activity regulated by the autonomic nervous system and can help diagnose conditions like small fiber neuropathy;
- Heart Rate Variability (“HRV”) Analysis, which assesses the variability in time between successive heartbeats, providing information about autonomic nervous system function;
- Blood tests may be performed to look for underlying causes of dysautonomia, such as testing for autoimmune markers, vitamin deficiencies, or thyroid function;
- Electrocardiogram (“ECG”), which measures the electrical activity of the heart and can reveal irregularities in heart rate and rhythm, which are common in certain dysautonomia conditions;
- Holter Monitor, a portable device that records the heart’s electrical activity continuously over a 24-48 hour period and can help identify intermittent heart rate abnormalities;
- Electromyography (“EMG”) and Nerve Conduction Studies, which evaluate nerve function and can help diagnose conditions that affect peripheral nerves, such as autonomic neuropathy;
- Gastric Emptying Study, which assesses the rate at which the stomach empties its contents and can be used to diagnose conditions like gastroparesis, a form of dysautonomia that affects digestion;
- Skin biopsy, which can be performed in cases of suspected small fiber neuropathy to examine the density of small nerve fibers in the skin;
- Imaging studies, such as magnetic resonance imaging (“MRI”) or computed tomography (“CT”) scans, may be used to evaluate the nervous system and rule out other conditions that could be contributing to symptoms;
- Doctor visit notes, including records of all visits you’ve made to your healthcare providers regarding your dysautonomia;
- Statements from your healthcare providers detailing the nature of your dysautonomia, your symptom and treatment history, and their opinion on your ability to work;
- Pharmacological records, including documentation of prescribed medications and treatments for symptom relief, along with any side effects or limitations these treatments may impose;
- Functional Capacity Evaluation (“FCE”), an assessment of your physical functioning which can objectively demonstrate the extent of your reduced functional capacity and work-related limitations caused by dysautonomia;
- Neuropsychological evaluation, which assesses how your condition affects your cognitive and mental functioning, providing your insurer comprehensive, objective data on cognitive impairments related to dysautonomia;
- “Bad News” Diary, a symptom journal you can keep detailing your day-to-day dysautonomia symptoms and how they impact your daily activities (including work); and
- Vocational evidence, including your resume, official job description from your employer, a personal affidavit describing the functions of your role and how your dysautonomia prevents you from meeting your job demands, witness statements from your employer or co-worker(s) describing how the onset of your dysautonomia impacted your job performance, and a vocational assessment from an expert analyzing whether you can perform the material duties of your occupation.
When seeking disability benefits for dysautonomia, it’s important to consult with an ERISA attorney who can help you compile the appropriate medical and vocational evidence. The strength of your claim largely depends on the quality and comprehensiveness of the medical and vocational evidence you present to demonstrate the disabling nature of your dysautonomia.
How can an attorney help me with my dysautonomia long term disability claim?
An experienced long term disability attorney can maximize your chances of getting your dysautonomia claim approved. At Riemer Hess, we’ve helped thousands of our clients secure their long term disability benefits, including many for conditions that cause dysautonomia. We understand what evidence your insurer will require to approve your claim and how to overcome the challenges inherent to disability claims for complex conditions like dysautonomia.
Here is an example of a client we helped secure long term disability for dysautonomia:
Our client “Jane,” a 40-year-old marketing manager, was a high-achiever known for her dedication. However, her life took an unexpected turn when she began experiencing dysautonomia. The symptoms began with occasional dizziness and fatigue, but over time, her condition worsened, affecting her ability to work effectively. Despite actively seeking treatment, Jane’s healthcare providers had not yet pinpointed a cause for her dysautonomia or found a treatment to manage her symptoms effectively. Her employers were supportive but couldn’t accommodate her for long.
Facing the reality that she could no longer work, Jane decided to explore a long term disability claim. She was very nervous about the prospect of her claim being denied, so she hired Riemer Hess to help her through the process.
Riemer Hess worked to gather extensive medical records on Jane’s behalf, including her doctor’s treatment notes, imaging studies, and blood test results. Understanding that her insurer would require more objective evidence of her dysautonomia, Riemer Hess referred Jane to undergo both a Tilt Table Test and a CPET evaluation. These test results provided objective and substantial evidence of the severity of her condition and its impact on her ability to work.
Riemer Hess ensured all documents were submitted correctly and on time, coordinating with Jane’s providers to obtain additional statements supporting her claim. When the insurer wanted to interview Jane by phone, our attorneys prepared her for the call and attended the call with her. Riemer Hess also helped answer the insurer’s questions about the ongoing treatment plan and prognosis.
Jane’s long term disability claim was approved, providing the financial stability she needed to cope with her condition. Jane was relieved to be receiving benefits and retained Riemer Hess to monitor her claim going forward.














